Coping With the Aftermath of Viral Infection
Understanding “Long-Haul” Covid
As if the initial infection wasn’t enough to have the world worried about COVID-19, there is now concern over the long-term effects of the disease. While the majority of patients recover unscathed from their Covid illness, a signifcant portion are reporting a wide array
of Covid “aftershocks.”
Long-Haul Covid or Long Covid refers to the lingering symptoms or other complications that many people experience months after being infected with the Coronavirus. And, it’s not just the respiratory system that is being affected. The CDC has created a list of symptoms associated with Long Covid.1 As time passes, we may find that more symptoms get added to this list. Dr. Anthony Fauci acknowledged this new crisis, stating that it “is really quite real and quite extensive.”
| The most commonly reported symptoms | Other reported symptoms | Less common but more severe complications that have been reported |
|
|
|
 At this point, we don’t know what percentage of those infected with the Coronavirus will experience long-term symptoms. Given the sheer number of infections, even if it is a small fraction, thousands upon thousands of people may continue to suffer long after the acute stage.
At this point, we don’t know what percentage of those infected with the Coronavirus will experience long-term symptoms. Given the sheer number of infections, even if it is a small fraction, thousands upon thousands of people may continue to suffer long after the acute stage.
Because the disease is so new, there are more questions among medical providers than there are answers. This is true for the practitioners here at Riordan Clinic as well. However, our extensive experience with other complex chronic illnesses (i.e. Epstein Barr, Lyme Disease, and others) may provide clues for successful Long-Haul Covid patient outcomes. As we begin seeing more of these patients, we can develop structured protocols for treatment.
Here’s what we do know – Chasing and treating symptoms is not enough.
We must also look at systemic weaknesses and other factors that prevent full recovery. As always, our approach is to eliminate any barriers to healing while also treating the condition at hand. Luckily we have many tools at our disposal that enable us to do this.
Lab Testing
Lab testing helps us gain valuable information about how the body is functioning. Particularly during times of illness or infection, optimal (not just “normal”) levels of nutrients are crucial. Vitamin D is a great example. Deficiency in vitamin D has been shown to increase susceptibility to infection. 2
We can make this vitamin on our own with proper sunlight exposure. However, our modern lifestyle, the ongoing quarantine, and cold winter temps keep us inside more often. Most people simply are not making enough. We can test for vitamin D and other nutrients to make sure the body has what it needs to not just function, but also fight infection and heal.
Lab testing can also give us information about inflammation, gut health, blood sugar, hormone balance, heavy metals, methylation factors, and other concerns that may alter the body’s ability to recover properly.
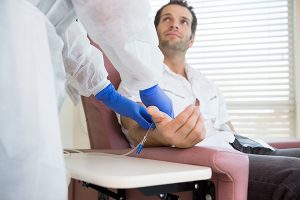 IV Vitamin C
IV Vitamin C
Vitamin C is a very potent antioxidant and plays a vital role in immune defense. When deficient in this vitamin, the body is more susceptible to infection.3 Additionally, infections quickly deplete the body of vitamin C due to inflammation and greater metabolic requirements. In cases such as Long-Haul Covid, oral supplementation may not be enough to replenish depleted stores.
Enter, IVC.
Intravenous Vitamin C enables the delivery of much larger doses, and it bypasses the digestive system for greater absorption and utilization.
Ultraviolet Blood Irradiation
Ultraviolet Blood Irradiation, or UBI for short, has been referred to as the “cure that time forgot.” It involves drawing a small amount of blood and processing it through a device that exposes it to controlled ultraviolet rays. Healthy cells remain unharmed, but most of the UV energy is absorbed by viral and bacterial cells. The diseased cells are killed and as a result, become antigenic. The treated blood is then returned to the body intravenously and creates a powerful immune response.
We have been using UBI at Riordan Clinic for several years for cases of chronic infection, inflammation, fibromyalgia, and autoimmune disorders.
Chelation
Chelation is a method of removing heavy metals from the body. Heavy metal toxicity, which can be a result of environmental exposure or ingestion, can have adverse effects on the immune response and interfere with enzyme function throughout the body, reducing a person’s ability to fight infection.
Medication (when needed)
Although we aim to treat disease with the most natural means possible, we also recognize that allopathic medicine has a time and place. There is promising research on certain medications for the prevention and treatment of Covid-19. When appropriate, medication may be used as part of a treatment plan.
Long-haul covid may look different for different people, and we are just beginning to understand the long-term implications of this illness. Based on the vast array of symptoms, it’s clear that it is more than just a respiratory disease.
The main point we want to drive home is this:
Do not ignore lingering (or new) symptoms that arise following a Covid-19 infection.
Seek treatment, uncover underlying barriers to your healing, and focus on getting well. We believe that the Riordan Approach will offer a more comprehensive pathway to resolution for Long Covid patients, and we are happy to help.
References:
https://www.cdc.gov/coronavirus/2019-ncov/long-term-effects.html?ACSTrackingID=USCDC_425-DM42580&ACSTrackingLabel=Weekly%20Summary%3A%20COVID-19%20Healthcare%20Quality%20and%20Worker%20Safety%20Information%20%E2%80%93%20November%2016%2C%202020&deliveryName=USCDC_425-DM42580
Aranow C. (2011). Vitamin D and the immune system. Journal of investigative medicine : the official publication of the American Federation for Clinical Research, 59(6), 881–886. https://doi.org/10.2310/JIM.0b013e31821b8755
Carr, A. C., & Maggini, S. (2017). Vitamin C and Immune Function. Nutrients, 9(11), 1211. https://doi.org/10.3390/nu9111211




